To read a PDF version of this report, click here.
Legislation introduced this month by U.S. Senators Bill Cassidy and Lindsey Graham combines most of the worst elements of earlier failed attempts to repeal and replace the Affordable Care Act.
The proposal would strip coverage from millions of Americans, raise costs for millions more (including those living with pre-existing conditions) and gut Medicaid – and it would harm New Jersey more than most other states.
- In all, about 2 million mostly low-income and vulnerable New Jerseyans would be significantly harmed by this proposal: 900,000[1] would likely lose their coverage entirely due to the cutbacks in the Medicaid expansion and Marketplace while the approximately 1.1 million additional New Jerseyans on Medicaid would be at risk of losing health coverage, benefits or access to medical services.
- New Jersey would lose about $5 billion[2] in federal funds each year, deepening the state’s budget crisis while devastating its economy – particularly its hospitals and health care sector, which would bleed tens of thousands of jobs as a result.
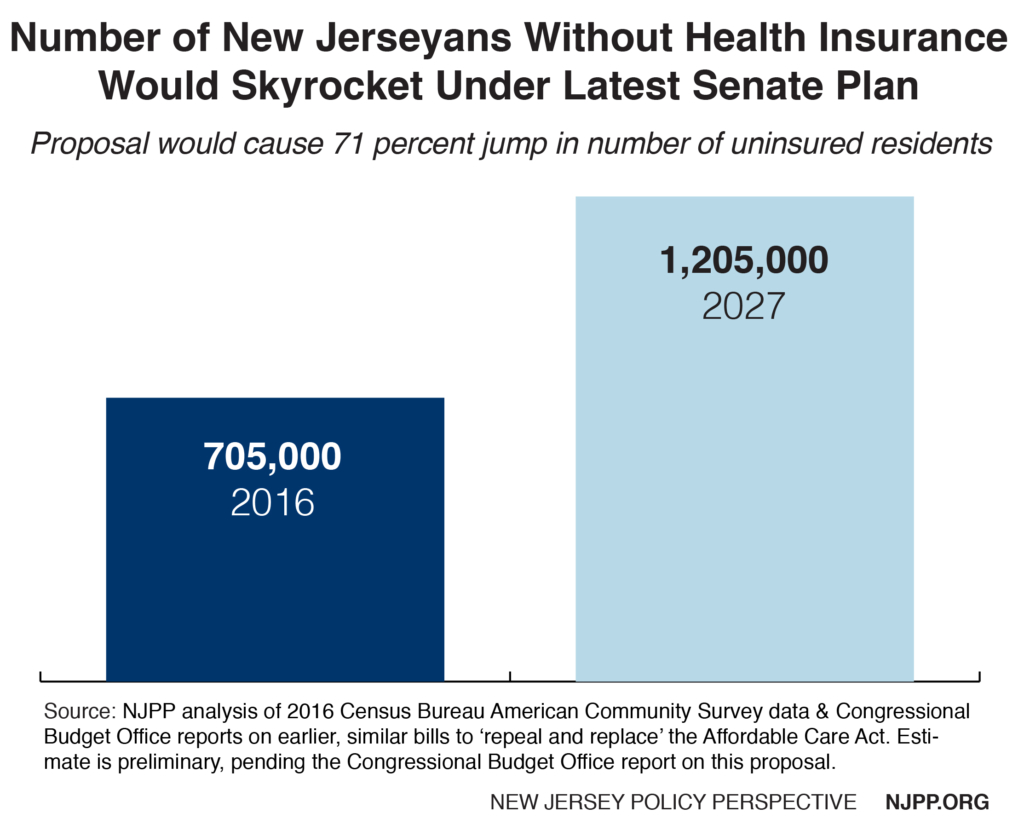
- The number of New Jerseyans without health insurance would skyrocket. An estimated 500,000 residents would become uninsured by 2027 – equaling an unprecedented 71 percent increase.[3] This would erase all the gains in health coverage New Jersey has made under the ACA, and leave the Garden State with 1.2 million uninsured residents. This would increase costs for local hospitals by $450 million, threatening their financial solvency.[4]
- New Jersey would also be hit hard because the bill redistributes millions of federal dollars from states that expanded Medicaid to those which did not to pick up more votes to pass the bill.
Elimination of Medicaid Expansion Would Cause Widespread Coverage Loss and Lead to Deep Cuts in Federal Funds
- Starting in 2020, this proposal turns the federal funding for the Medicaid expansion into a block grant before eliminating funding altogether in 2027. This would likely result in all of the 540,000 New Jerseyans who’ve currently obtained coverage under the expansion to lose it by 2027.
- By 2027, New Jersey would be losing about $4 billion in federal funds each year, eliminating a major source of funding for the state’s campaign to treat opioid addicts.[5]
Radical Medicaid Changes Put Over a Million New Jerseyans at Risk
- Like earlier proposals, this one would result in lost or reduced health care for an additional 1.1 million[6] New Jerseyans due to a permanent cap on Medicaid that would drastically reduce funding to New Jersey.
- New Jersey would lose about $4.4 billion in federal funds between 2020 and 2026 under this cap.[7] The amount would skyrocket after 2026 due to changes in the way the cap is calculated.
- New Jersey’s seniors and people with disabilities would be most at risk because they account for 64 percent of all Medicaid expenditures in the state.[8]
- Prescription drug coverage, community-based care for seniors and people with disabilities, and dental coverage would be especially vulnerable to elimination because they are considered optional in Medicaid.
Marketplace Insurance Would be Unaffordable for Nearly Everyone
- Starting in 2020, up to 200,000[9] New Jerseyans would begin to lose their insurance in the individual Marketplace due to the elimination of the individual mandate and phase out of all subsidies. These subsidies would be temporarily converted to an inadequate block grant from the federal government to states but by 2027 funding for this crucial tool to help keep insurance affordable would disappear. New Jersey would lose about $1 billion in federal funds for subsidies each year starting in 2027.[10]
- An additional 150,000[11] New Jerseyans who don’t receive subsidies would either lose private health coverage or have to pay much more for it, because the state’s insurance premiums would likely return to the highest level in the nation (as they were before the ACA).
Protections for New Jerseyans With Pre-Existing Conditions & Coverage for Essential Health Services Could Disappear
- The latest proposal allows states to opt out of ACA protections that prevent insurers from charging higher premiums based on health status, jeopardizing affordable coverage for millions of New Jerseyans with pre-existing conditions.
- It also allows states to opt out of ACA requirements that insurers cover essential health benefits like hospitalization, maternal care and treatment for substance abuse; this could also harm many of the 5 million New Jerseyans who have employer-based insurance.
Endnotes
[1] Consists of 600,000 New Jerseyans who are projected to be in the Medicaid expansion by 2027, 200,000 who are projected to receive Marketplace subsidies and 100,000 who do not receive subsidies and would drop their individual insurance because it would be unaffordable.
[2] Includes all federal funding lost in Marketplace subsidies and the Medicaid expansion
[3] NJPP analysis of 2016 Census Bureau American Community Survey data & Congressional Budget Office reports on earlier, similar bills to ‘repeal and replace’ the Affordable Care Act. Estimate is preliminary, pending the Congressional Budget Office report on this proposal.
[4] Kellogg Insight, Who Bears the Cost of the Uninsured? Nonprofit Hospitals, June 2015. https://insight.kellogg.northwestern.edu/article/who-bears-the-cost-of-the-uninsured-nonprofit-hospitals
[5] NJPP analysis of New Jersey Department of Human Services data on Medicaid expansion expenditures submitted to the Office of Legislative Services for the 2018 budget, adjusted for inflation. http://www.njleg.state.nj.us/legislativepub/budget_2018/DHS_response.pdf
[6] New Jersey Division of Medical Assistance and Health Services Enrollment Reports, excluding CHIP. http://www.state.nj.us/humanservices/dmahs/news/reports/index.html
[7] Center on Budget and Policy Priorities, Like Other ACA Repeal Bills, Cassidy-Graham Plan Would Add Millions to Uninsured, Destabilize Individual Market, September 2017. https://www.cbpp.org/research/health/like-other-aca-repeal-bills-cassidy-graham-plan-would-add-millions-to-uninsured
[8] Kaiser Family Foundation, Medicaid Spending by Enrollment Groups, 2014.
[9] U.S. Department of Health and Human Services, Assistant Secretary for Planning and Evaluation, Compilation of State Data, 2016, https://aspe.hhs.gov/compilation-state-data-affordable-care-act
[10] Ibid. Includes $166 million for cost sharing subsidies and $792 million for premium subsidies.
[11] NJ Department of Banking and Insurance, Individual Health Coverage Program, 1Q2017, http://www.state.nj.us/dobi/division_insurance/ihcseh/enroll/1q17ihcmarket.pdf